Understanding the intricacies of medical equipment is crucial for healthcare professionals. The question often arises: "what is the difference between respiratory and anesthesia systems?" Dr. Emma Thompson, a leading expert in anesthesia management, notes, "Both systems serve vital roles, yet their functions are distinctly different."
Respiratory systems focus on facilitating normal breathing for patients, particularly those with lung conditions. These systems include ventilators that support or replace spontaneous breathing. On the other hand, anesthesia systems are designed specifically to deliver anesthetic agents during surgical procedures, ensuring patient safety and comfort. Anesthesia systems combine gases and monitors to maintain consciousness levels.
Misunderstanding these systems can lead to serious consequences. It is easy to confuse their roles, especially in high-pressure situations. While respiratory systems assist with breathing, anesthesia systems are critical for sedation and pain management. Distinguishing between the two requires a strong foundation in their principles. Continued education is necessary for those in the field. Always reflect on the specific needs of each patient to ensure the correct system is used.
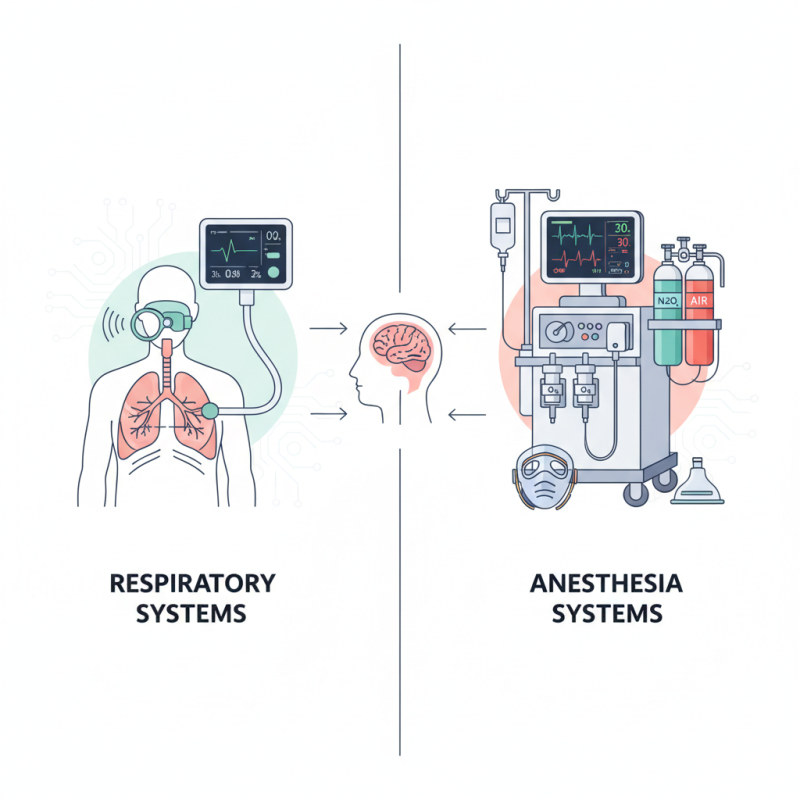
Understanding the basics of respiratory and anesthesia systems is crucial for medical professionals. These systems play vital roles in patient care during surgeries and respiratory interventions. A respiratory system provides oxygen and removes carbon dioxide. In contrast, a anesthesia system manages the delivery of anesthetic agents for sedation.
Respiratory systems include components like ventilators, humidifiers, and oxygen tanks. Each part must function correctly to support a patient’s breathing. Anesthesia systems typically have gas cylinders, vaporizers, and monitoring devices. These systems require precise calibration and regular maintenance. Medical staff must be proficient in using these tools. Mismanagement can lead to severe complications.
While both systems serve distinct purposes, their operation occasionally overlaps. They share some common components, like monitors and tubing. Understanding this connection is essential but can be challenging. Continuous education is necessary to improve proficiency. Reflecting on experiences helps identify areas for growth.
In clinical settings, the respiratory system plays a crucial role in patient care. Understanding its key components can enhance effective interventions. Essential elements include ventilators, nebulizers, and oxygen delivery devices. Each component serves a specific purpose in maintaining optimal respiratory function. Ventilators provide mechanical assistance to patients who cannot breathe adequately. They come with various modes that allow clinicians to tailor support to individual needs.
When using nebulizers, accuracy in medication delivery is vital. This device converts liquid medication into a mist, ensuring patients receive their treatment effectively. Proper maintenance is crucial to prevent contamination. Clean the device regularly and check for blockages to ensure efficient operation.
**Tips:**
Ensure that oxygen therapy is titrated carefully based on patient response. Monitor saturation levels consistently. Remember, over-supplying oxygen can lead to complications. Always assess each patient’s unique requirements and adjust accordingly.
While these components are critical, the integration of technology complicates things. New devices emerge frequently, which can be overwhelming. It’s important to stay updated through training, workshops, and peer consultation. This knowledge helps in making informed decisions for better patient outcomes.
Anesthesia delivery systems are crucial in medical environments. They ensure patient safety and comfort during procedures. Essential features of these systems include reliable gas delivery, precise monitoring, and efficient vaporization of anesthetic agents. According to the American Society of Anesthesiologists, over 50 million surgeries requiring anesthesia are performed annually in the United States alone.
A well-designed anesthesia system incorporates advanced safety mechanisms. These include pressure relief valves and alarms. As reported by the World Health Organization, equipment failures can lead to serious complications. Understanding these features is key for healthcare professionals. The unique design aspects help differentiate anesthesia systems from simple respiratory equipment.
Tip 1: Always check calibrations before use. Small discrepancies can lead to significant errors.
It’s vital to consider training and knowledge in using these systems. Inadequate training can compromise patient safety. Continuous education ensures practitioners are updated on best practices.
Tip 2: Stay informed on the latest safety guidelines. Changes in protocols can arise frequently.
Customizing the approach based on each patient's needs is essential. Consider factors like age and health status, as they impact anesthetic requirements. Each case demands careful assessment to create the best outcome.
Differentiating between respiratory and anesthesia systems is crucial in clinical settings. While both systems aim to ensure proper oxygenation, their functions differ significantly. Respiratory systems focus on the patient's breathing. They provide the necessary support for ventilation, ensuring that oxygen reaches the lungs effectively.
Anesthesia systems, on the other hand, are more complex. They not only control ventilation but also manage the delivery of anesthetic agents. This is vital during surgeries, where patient awareness and pain are minimized. The presence of monitoring devices is commonplace in these systems. They track vital signs, ensuring patient safety throughout procedures.
Understanding these differences is essential for healthcare professionals. It’s important to recognize that despite their overlapping functions, the intended outcomes differ. Respiratory systems are about sustaining life, while anesthesia systems prepare patients for interventions. Misunderstandings can lead to serious consequences, making awareness a key component of effective care.
| Feature | Respiratory System | Anesthesia System |
|---|---|---|
| Primary Function | Gas exchange, oxygen delivery | Induction and maintenance of anesthesia |
| Components | Ventilator, humidifier, oxygen supply | Vaporizer, breathing system, monitoring devices |
| Monitoring | Lung function, oxygen saturation | Depth of anesthesia, vital signs |
| Typical Usage | Critical care, chronic respiratory conditions | Surgical procedures requiring anesthesia |
| User Interface | Less complex, focused on ventilation settings | More complex, with multiple anesthesia parameters |
Differentiating respiratory and anesthesia systems is crucial for patient care. Each system serves distinct purposes, impacting clinical outcomes. According to a report by the American Society of Anesthesiologists, over 30% of anesthesia-related complications stem from miscommunication about equipment functions. Understanding these differences can reduce risks significantly.
In respiratory systems, focus on ventilation and gas exchange. Examples include ventilators and CPAP machines. These devices monitor respiratory rates and oxygen levels closely. In contrast, anesthesia systems concentrate on delivering anesthetic agents. They require precise dosing and monitoring for safety. A study published in Anesthesiology found that improper machine adjustments could lead to hypoxia or overdose.
Tip: Always verify machine settings before use. Regular training helps staff remain updated on system nuances.
Irregularities in system performance can compromise patient safety. Routine maintenance is essential. Studies show that approximately 15% of equipment failures occur due to lack of servicing. Teams need streamlined communication to ensure device efficacy.
Tip: Maintain a checklist for equipment readiness. This small step can enhance patient outcomes.
: Respiratory systems provide oxygen and remove carbon dioxide from the body.
Anesthesia systems ensure patient safety and comfort during surgical procedures.
Key components include ventilators, nebulizers, and oxygen delivery devices.
Ventilators offer mechanical assistance to patients who struggle to breathe on their own.
Regular cleaning prevents contamination and ensures effective medication delivery.
Over-supplying oxygen can lead to serious complications in patients.
New devices frequently emerge, making it essential to stay updated through training.
Always check calibrations, as small errors can cause significant issues.
Ongoing training ensures staff are aware of best practices and safety guidelines.
Factors like patient age and health status impact individual anesthetic requirements.
The article "2026 How to Differentiate Respiratory and Anesthesia Systems?" explores the fundamental aspects that distinguish respiratory systems from anesthesia systems in a clinical context. Understanding the basics involves recognizing that respiratory systems primarily facilitate gas exchange and support ventilation, while anesthesia systems are designed to administer anesthetic agents and monitor vital signs during surgical procedures.
Key components of respiratory systems include ventilators and oxygen delivery devices, whereas anesthesia delivery systems incorporate vaporizers and flowmeters. The critical differences between respiratory and anesthesia functions lie not only in their components but also in their applications in patient care. This comparative analysis highlights that a clear understanding of what is the difference between respiratory and anesthesia systems is essential for healthcare professionals to provide optimal care and ensure patient safety during various medical interventions.

 Ryu Medical
Ryu Medical