In the healthcare sector, sterile medical tubing plays a crucial role. Dr. James H. McCarthy, a leading expert in medical device safety, emphasizes, "Sterile medical tubing is vital for preventing infection in patients." Understanding why is sterile medical tubing important involves examining its role in both patient safety and healthcare efficiency.
Sterile medical tubing is used in various procedures, from IV deliveries to surgical operations. This tubing must remain free from contaminants to protect vulnerable patients. A lapse in sterility can lead to severe infections or complications. Therefore, maintaining high standards in production and handling is essential.
The pressure to ensure sterility can sometimes lead to oversight. For instance, facilities might prioritize speed over stringent sterilization processes. This reflects a critical challenge faced by healthcare providers today. As we navigate these complexities, the need for reliable sterile medical tubing becomes even more apparent.
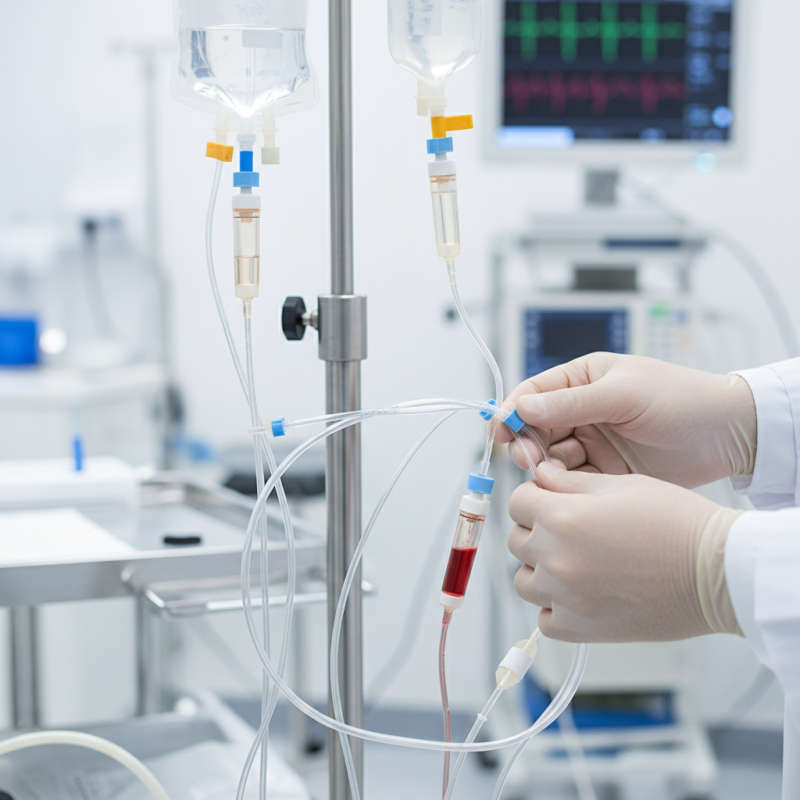
Sterile medical tubing plays a crucial role in healthcare settings. It acts as a barrier against harmful pathogens. When procedures involve invasive techniques, the risk of infection increases. Using sterile tubing helps to mitigate this risk significantly. In surgery, for instance, any slight contamination can lead to severe complications. Proper sterilization reduces this risk, protecting patients from potential infections.
During fluid transfer, the integrity of the tubing is critical. If the tubing is compromised, contaminants can easily enter. Healthcare professionals must ensure strict adherence to sterilization protocols. This often includes rigorous testing and inspection before use. Small oversights can lead to dire consequences, highlighting the need for diligence. Each piece of tubing must be treated with care to promote patient safety.
Moreover, challenges in maintaining sterility remain. False confidence can arise when protocols are not followed correctly. Regular training for staff is essential to instill this importance. As we strive for better hygiene practices, recognizing potential flaws in the system becomes vital. Medical tubing may seem simple, but its impact is profound within patient care. A lapse in protocol can result in infections, urging constant evaluation of best practices.
Sterile medical tubing is crucial in various healthcare contexts. Its primary role is in surgical procedures, where infection control is paramount. According to the Global Market Insights report, the sterile medical tubing market is expected to surpass $7 billion by 2026. This reflects the growing demand for safe and efficient healthcare practices.
In hospitals, sterile tubing is used in intravenous (IV) therapy and respiratory care. For example, during surgeries, it is vital for ensuring that fluids and medications are delivered directly to patients without contamination. Additionally, sterile tubing is integral in medical devices like catheters and feeding tubes. The Centers for Disease Control and Prevention emphasize the importance of using sterile equipment to minimize infection risks.
Yet, challenges remain in maintaining strict sterile protocols. Even minor lapses can lead to significant health risks. A 2018 study highlighted that approximately 24% of healthcare-associated infections were linked to improper tubing practices. Continuous training and adherence to guidelines are essential for healthcare professionals to mitigate these risks. Being aware of potential pitfalls is critical in driving improvements in patient safety.
Sterile medical tubing plays a crucial role in healthcare. The material used in these tubes can significantly impact patient safety. Various materials, such as PVC, silicone, and polyurethane, have unique benefits and shortcomings. According to industry reports, over 70% of hospitals use PVC for its affordability, but concerns over plasticizers have emerged.
Silicone provides excellent biocompatibility, making it suitable for long-term use. However, its higher cost limits widespread adoption. Polyurethane is another option; it combines strength and flexibility, yet it requires careful handling during sterilization processes. The choice of material can influence the effectiveness of sterilization and the risk of contamination.
Tips: Always review the material specifications before choosing medical tubing. Sterility alone does not guarantee safety; ongoing assessments are needed. Engaging with healthcare professionals about material preferences and limitations can provide insights that enhance safety measures. Consider the environment; some materials have larger carbon footprints. Aim for balance between performance and sustainability.
Sterile medical tubing plays a critical role in healthcare. Ensuring patient safety hinges on the compliance of these products with strict regulatory standards. Production methods must adhere to guidelines established by organizations such as the FDA and ISO. In the U.S., for instance, FDA regulations mandate that manufacturers follow Good Manufacturing Practices (GMP). These requirements help ensure that the tubing is free from contaminants.
Data from the Global Industry Analysts report emphasizes that the sterile medical tubing market is projected to reach over $5 billion by 2025. Such growth highlights the increasing demand for safe and reliable medical devices. However, not all manufacturers meet these high standards, leading to concerns about product integrity. The variability in compliance can lead to inflated healthcare costs and increased risks for patients.
Quality assurance is essential. Testing standards, such as sterility assurance levels (SAL), dictate the methodologies used in sterilization. These methodologies must be validated regularly to reduce risks. Despite advancements, there are still instances of contamination. Continuous monitoring and improvement of production processes should be prioritized. The healthcare industry must remain vigilant to uphold the highest standards.
Maintaining sterility in medical tubing is crucial for patient safety. Contaminated tubing can lead to severe infections, increased hospital stays, and higher healthcare costs. According to the Centers for Disease Control and Prevention (CDC), healthcare-associated infections (HAIs) affect one in every 31 hospital patients on any given day. This statistic highlights the importance of strict protocols for sterilizing medical equipment, including tubing.
One of the key challenges in maintaining sterility is human handling. A study published in the Journal of Hospital Infection found that 15% of surgical instrument sets were contaminated at the time of use. This contamination risk extends to tubing during transport and storage. Improper storage conditions can promote bacterial growth. If facilities do not adhere to sterilization guidelines, the risk of infection increases significantly.
Another issue arises from the materials used for tubing. Certain types can be more susceptible to biofilm formation, which poses a serious health risk. Research indicates that biofilms on medical devices are responsible for over 80% of microbial infections. Regular training and updates on best practices can help address these challenges, ensuring that healthcare professionals remain vigilant in their efforts to maintain sterility in medical tubing.
: It serves as a barrier against harmful pathogens during invasive procedures, reducing infection risk.
Contaminants can enter, increasing the likelihood of severe complications and infections for patients.
By adhering to strict sterilization protocols, conducting rigorous testing, and inspecting tubing before use.
Small lapses in sterilization protocols or handling can have serious consequences, leading to patient safety risks.
Human handling can introduce contamination, making proper training essential for healthcare staff.
It can promote bacterial growth, increasing the risk of infection if guidelines are not followed.
Biofilms can lead to over 80% of microbial infections, making material selection and care critical.
Regular updates are necessary to ensure professionals remain vigilant in maintaining sterilization compliance.
They can result in severe infections, extended hospital stays, and higher healthcare costs for patients.
Continuous evaluation of practices, ongoing vigilance, and recognition of potential system flaws are essential.
Sterile medical tubing plays a crucial role in healthcare by preventing infections that can arise from contaminated equipment. Understanding why sterile medical tubing is important involves recognizing its key applications in various medical procedures, from intravenous therapies to surgical interventions. The choice of materials used in manufacturing this tubing is vital to ensure compatibility, strength, and safety, thus impacting patient outcomes.
Regulatory standards are in place to govern the production of sterile medical tubing, ensuring that healthcare providers can rely on these tools to be safe and effective. However, challenges remain in maintaining sterility during usage, which requires stringent protocols and proper handling techniques. Overall, the significance of sterile medical tubing in healthcare cannot be overstated, as it is essential for delivering safe and effective patient care.

 Ryu Medical
Ryu Medical